You have done physical therapy, medications, injections, or even surgery.
You already have an MRI.
You have a diagnosis.
Maybe you were told:
You have a disc bulge.
Spinal stenosis.
Degenerative disc disease.
Yet you still hurt.
Persistent back or spine pain is often treated with therapy, medication, injections, or surgery.
When symptoms continue, the issue is frequently that the true source of pain has not been clearly identified.
static Imaging findings alone do not always reflect the primary pain source.
Many treatments are directed toward the most obvious finding.
Sometimes that works.
Sometimes it doesn’t.
When symptoms persist despite therapy, injections, medications, or surgery, it raises an important question:
Was the correct structure ever being treated?
The answer is not always obvious.
Pain may originate from discs, facet joints, sacroiliac joints, ligaments, muscles, peripheral nerves, or multiple pain generators acting together.
Pain may originate from discs, facet joints, sacroiliac joints, ligaments, muscles, peripheral nerves, or multiple pain generators acting together.
Back pain rarely originates from a single structure.
Evaluation focuses on identifying what is actually producing symptoms rather than simply cataloging abnormalities.
Review of imaging, detailed physical examination, diagnostic reasoning, dynamic assessment, and ultrasound-guided evaluation are used to guide treatmenrt.
The goal is clarity.
Because treatment becomes much more precise once the pain source is identified.
Treatment depends on what is found during evaluation.
For some patients, improvement may require rehabilitation, movement modification, strength restoration, or biomechanical correction.
For others, image-guided diagnostic injections, precision spine procedures, regenerative therapies, or other targeted interventions may be considered.
Treatment follows diagnosis.
Not the other way around.
Treatment decisions are individualized and guided by clinical findings, imaging correlation, functional limitations, and long-term spine health rather than predetermined protocols.
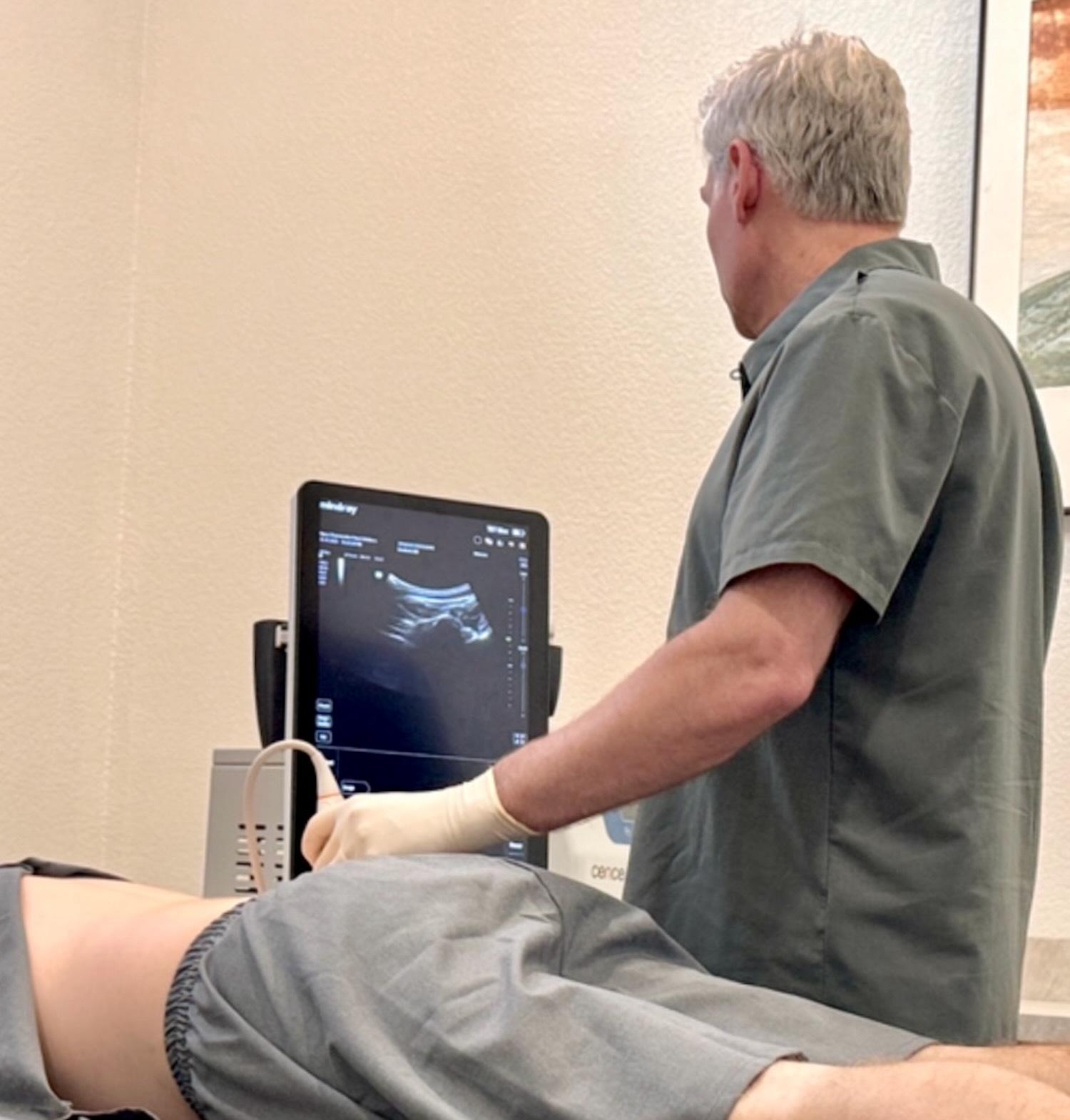
Image-guided spine injections may be used diagnostically or therapeutically to clarify and address specific pain generators.
These may include epidural steroid injection for radicular symptoms, facet joint injections, medial branch blocks, or sacroiliac joint injections when clinically indicated.
The goal of interventional care is diagnostic clarity and targeted relief — not indiscriminate procedural escalation.
In selected cases, regenerative medicine approaches may be considered for facet joint–related pain, sacroiliac joint dysfunction, or carefully evaluated disc-related conditions.
Platelet-Rich Plasma (PRP) and other autologous biologic therapies may be discussed when appropriate within a broader spine care strategy.
These options are considered only after thorough evaluation and discussion of realistic expectations, with emphasis on structural stability and long-term functional improvement.
Persistent or function-limiting spine pain deserves careful structured evaluation.
Whether symptoms are recent or longstanding, a comprehensive physician consultation helps clarify diagnosis and appropriate next steps.
Care begins with understanding the spine in motion and in context — not simply interpreting imaging findings in isolation.
If you're unsure whether your spine or back pain is appropriate for this approach, you may text directly to discuss your situation.
Text Dr. Bernhardt